10 Best Things You Should Know About Knee Replacement Surgery?
Knee replacement surgery is a significant medical procedure that impacts countless lives each year. In the United States alone, approximately 800,000 knee replacements are performed annually, as reported by the American Academy of Orthopaedic Surgeons. This surgery aims to relieve pain, improve functionality, and enhance the quality of life for those suffering from severe knee damage due to conditions like osteoarthritis. Understanding key aspects about knee replacement surgery can empower patients to make informed decisions.
Despite its benefits, patients should be aware of potential drawbacks. Some individuals may experience complications, such as infection or blood clots, with a 1% to 2% incidence rate, according to a 2021 study published in the Journal of Bone and Joint Surgery. It is vital for patients to discuss their specific risks with their healthcare providers. Additionally, the recovery process can be demanding and varies for each person, often requiring physical therapy and lifestyle adjustments.
For those considering this procedure, informed choices lead to better outcomes. Staying well-informed includes understanding the procedure, recovery expectations, and potential risks. Research has shown that patients who engage actively in their treatment plans tend to achieve better results. Thus, exploring the ten best things about knee replacement surgery can provide valuable insights for prospective patients.

Understanding Knee Replacement Surgery: An Overview
Knee replacement surgery is a significant procedure that can alleviate pain and improve mobility. Many patients consider it when conservative treatments fail. It involves replacing damaged or worn-out knee joints with artificial components. Understanding the process is crucial for potential candidates.
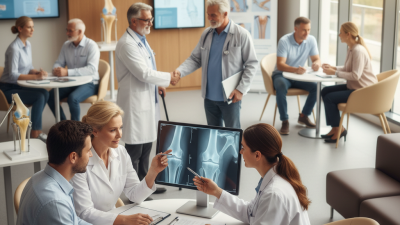
Preparation is key. Before surgery, consult with a qualified orthopedic surgeon. They can assess your condition and determine the best approach. Discuss your medical history and any concerns. This conversation builds trust and ensures you are fully informed.
Recovery may vary. Patients often face challenges like pain management and rehabilitation. It’s vital to follow your doctor’s post-operative guidelines. Start physical therapy early, as it can help you regain strength and mobility. Remember, progress can be slow. Some days may feel frustrating, but persistence is essential.
Tips: Stay active during recovery. Light activities, like walking, can prevent stiffness. Hydration and a balanced diet also support healing. Don’t hesitate to ask for help when needed. Having a support system can make a difference, as the emotional journey is as important as the physical one.
10 Best Things You Should Know About Knee Replacement Surgery
Types of Knee Replacement Procedures Available
Knee replacement surgery has evolved significantly over the years. Today, there are mainly two types of procedures: total knee replacement (TKR) and partial knee replacement (PKR). Total knee replacement involves replacing the entire joint, while partial knee replacement focuses on only the damaged part. According to the American Academy of Orthopaedic Surgeons, about 700,000 total knee replacements are performed each year in the United States.
For patients with arthritis mainly affecting one side of the knee, PKR can be a suitable option. Data from the Journal of Orthopaedic Surgery and Research indicates that PKR patients often experience less pain and a quicker recovery. However, not everyone is a candidate for this procedure. Some studies show that about 20% of PKR patients may require a conversion to TKR later. This highlights the importance of thorough pre-operative assessments.
Moreover, robotic-assisted knee replacements have emerged as a promising technique. Research from the Journal of Bone and Joint Surgery suggests that this approach may improve precision and outcomes. However, the technology often comes with higher costs and varied availability. Understanding these options and their implications is essential for making informed decisions about knee surgeries.
Common Indications for Knee Replacement Surgery
Knee replacement surgery is often recommended for patients experiencing severe knee pain and dysfunction. Common indications include osteoarthritis, rheumatoid arthritis, and post-traumatic arthritis. Osteoarthritis, the most prevalent reason, results from wear and tear on the joint. This condition causes significant pain and limits mobility.
Rheumatoid arthritis affects the lining of the joints, leading to painful swelling. Patients may experience stiffness that makes daily activities challenging. Post-traumatic arthritis can arise from previous injuries to the knee, which may create long-term damage. Evaluating the severity of these conditions is crucial in determining the necessity for surgery.
However, surgery should not be the first choice. Physical therapy and lifestyle adjustments can be initial steps. Patients often express anxiety about recovery times and the risks involved. Conversations with orthopedic specialists can provide clarity. Understanding the benefits, risks, and realistic outcomes is essential for making informed decisions, ensuring the surgery aligns with patient expectations and needs.
10 Best Things You Should Know About Knee Replacement Surgery
| Indication | Description | Typical Age Range for Surgery | Success Rate (%) |
|---|---|---|---|
| Severe Osteoarthritis | Degeneration of cartilage causing pain and stiffness. | 50-80 years | 90% |
| Rheumatoid Arthritis | Autoimmune disorder leading to joint pain and inflammation. | 40-70 years | 85% |
| Post-Traumatic Arthritis | Arthritis resulting from injury to the knee joint. | 30-60 years | 80% |
| Knee Deformities | Congenital or acquired deformities causing pain. | All ages | 75% |
| Avascular Necrosis | Loss of blood supply to the bone, causing degeneration. | 30-50 years | 70% |
| Failed Previous Surgery | Complications or unmet expectations from prior knee surgeries. | 40-70 years | 80% |
| Chronic Knee Pain | Persistent pain despite non-surgical treatments. | All ages | 85% |
| Infection in the Joint | Infections that affect the knee, requiring joint replacement. | All ages | 75% |
| Recurrent Joint Effusion | Frequent swelling and buildup of fluid in the knee joint. | 40-60 years | 80% |
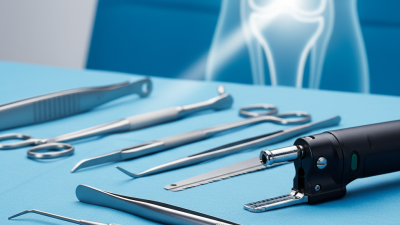
The Surgical Process: What to Expect on Surgery Day
Knee replacement surgery is a significant event. Knowing what to expect can ease anxiety. On surgery day, patients typically arrive early. Medical staff will greet you and prepare for the procedure. You’ll meet the surgical team, ensuring everyone is on the same page.
After checking in, you’ll change into a hospital gown. An IV will be placed in your arm for fluids and medications. Some patients feel nervous at this stage. It’s okay to express your feelings. Nurses will guide you through the process. Expect to receive anesthesia before surgery. This will make you numb or put you to sleep.
Once in the operating room, the environment will be busy. Team members will verify your details and start the procedure. You might feel a little disoriented. It’s normal to experience a mix of excitement and fear. Ultimately, the focus is on your safety and health. Remember, it's a step toward relieving pain and regaining mobility.
Post-Operative Care and Rehabilitation for Knee Replacement

Post-operative care and rehabilitation are critical for successful knee replacement surgery outcomes. Approximately 90% of patients experience significant relief from pain and improved mobility after the procedure, according to recent studies. However, recovery can vary considerably among individuals. Effective rehabilitation begins in the hospital. Within 24 hours post-surgery, physical therapy usually starts, focusing on gentle range-of-motion exercises. These early activities help reduce complications and promote healing.
Home care is equally vital after discharge. Patients must adhere to a prescribed exercise regimen, typically including quadriceps and hamstring strengthening. The American Association of Orthopaedic Surgeons suggests that routine physical therapy sessions can enhance recovery speed and functional outcomes. A study revealed that patients engaged in guided physical therapy were more likely to regain their pre-surgery activity levels.
Despite best efforts, some patients may struggle with rehabilitation. Pain management, swelling, and mobility issues can hinder progress. Observing prescribed rest and activity limitations is essential, but some may push themselves too hard. The road to recovery is often filled with challenges, requiring patience and commitment from both patients and healthcare providers. Regular follow-ups with the surgeon can help address setbacks and ensure the rehabilitation path is adjusted as needed.